Tension Free Vaginal Tape (TVT)
The goal of surgery for stress urinary incontinence is to stop urinary leakage and this is accomplished by supporting the urethra. The urethra is the tube that allows urine to be expelled from the body. In an attempt to support the urethra, the vagina under and beside the urethra is the area which the operation takes place. This procedure is commonly called the SLING.
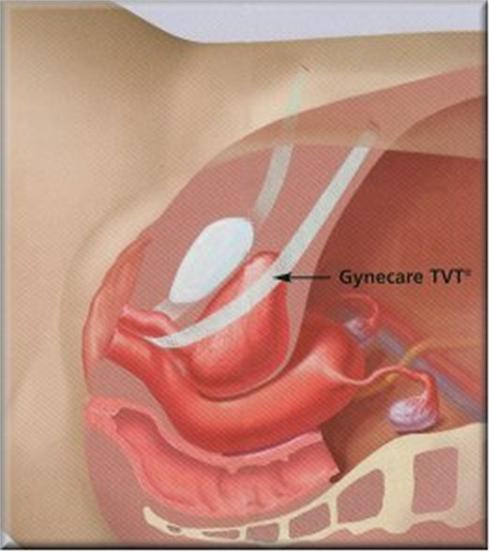
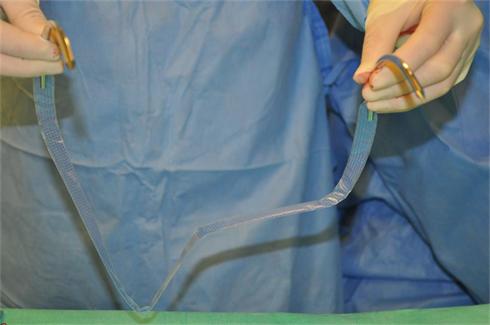
The operation has the following advantages:
-
Minimally invasive (two incisions of 1/3 inch on the pubic hairline
-
Minimal pain (40% of patients will not need a pain reliever after 24 hours)
-
Proven cure rate of 86%
-
Same day or next day discharge for 98% of patients
-
Performed under local anesthesia and IV sedation
-
Operative time 20-30 minutes Minimal postoperative need for catheterization
-
Minimal complications which include voiding dysfunction, mesh erosion and urinary urgency
For further information about recovery following surgery, please visit www.rcog.org.uk/ recovering-well, and click on mid urethral sling procedures laparoscopy
Mesh Vaginal Repairs
Mr Fayyad is one of few urogynaecologists in the UK performing mesh vaginal repairs for women with prolapse. Generally, the current indication is in women with recurrent prolapse (i.e. had previous prolapse treatment that did not work). Mr Fayyad uses the Prolift Total Mesh System in this select group of patients. Mr Fayyad has published his own experience in the use of this mesh system which is the longest follow up study currently published.
Posterior Prolift
For further information about recovery following surgery, please visit www.rcog.org.uk/ recovering-well, and click on pelvic floor repair.
Laparoscopic Uterine Suspension (Laparoscopic sacrohysteropexy)
Traditional medicine recommends removal of the uterus (hysterectomy) when there is uterine prolapse. In cases of severe uterine and vaginal prolapse a hysterectomy followed by vaginal wall reconstruction may still be the most beneficial therapy. However there are more women who are electing to keep their uterus especially in those whom the uterus is only mildly or moderately prolapsed. The decision to attempt uterine and vaginal support is made only after a full informed consent is made with the patient having the operation. One of the most important aspects of this surgery is the lack of long term data supporting its utilization in uterine and vaginal prolapse surgery.
There are many methods of uterine suspension including sacrospinous tailbone) and uterosacral ligament suspension. Mr Fayyad routinely performs the laparoscopic approach and/or utilizing mesh to suspend the uterus (sacrohysteropexy Figures 1 and 2) or in some cases the uterosacral ligaments.
In the laparoscopic sacrohysteropexy with mesh, The cervix is grasped by special forceps (Figure 3). An incision is then made in the vaginal skin surrounding the cervix and a soft nylon mesh is then sutured to the cervix (Figure 4) and the vaginal skin closed over it (figure 5). The mesh is then secured to the sacrum (tailbone) through key-hole surgery (Figure 6) after reducing the prolapsed uterus. Then mesh is then buried using laparoscopic suturing techniques (Figure 8).
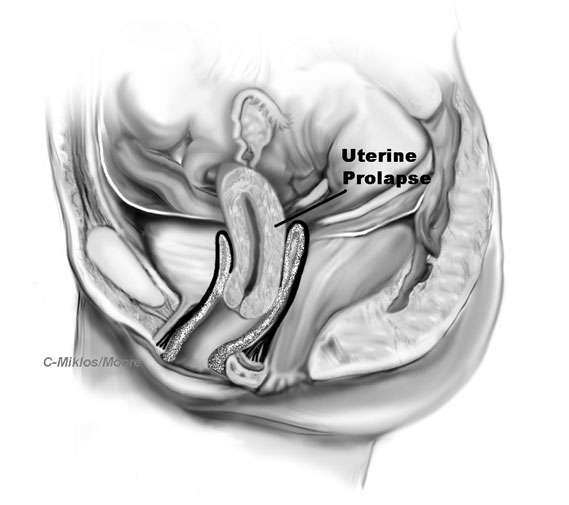
Figure 1: Diagrammatic presentation of uterine prolapse
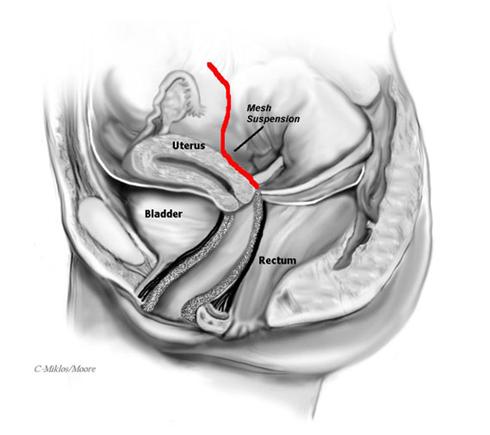
Figure 2: Sacrohysteropexy with mesh attaching the cervix to the sacrum.
Vaginal Vault Suspension (Laparoscopic Sacrocolpopexy)
Overview
Vaginal vault prolapse occurs when the apex of the vagina (upper 1/3 of the vagina) has broken away from its original support structure known as the uterosacral ligaments. The uterosacral ligaments hold up the apex and the uterus when the uterus is in place (Figure 1). When a patient has a hysterectomy, the uterosacral ligaments must be cut to remove the uterus. In an attempt at preventing future vaginal apex or vault prolapse, the uterosacral ligaments should be attached to the apex of the vagina after the uterus has been removed.
If the patient did not have her uterosacral ligament attached to the vaginal apex or the uterosacral ligaments did not remain attached after the surgery, the patient risks ending up with vaginal vault prolapse after the hysterectomy (Figure 2). As the prolapse continues to pull down, it will increase the risk of anterior and posterior paravaginal defects.

Figure 1 Uterine & vaginal vault prolapse - The uterus begins to prolapse because of the broken uterosacral ligament.
IT IS VITAL THAT A VAGINAL VAULT SUSPENSION BE COMPLETED AT THE TIME OF PROLAPSE SURGERY IF VAULT PROLAPSE IS EVIDENT, WHICH IN MANY CASES IT IS.
Vaginal vault prolapse can also occur in many patients months or years after a hysterectomy in conjunction with other pelvic floor defects such as cystocele, rectocele, or enterocele. It is very important that the surgeon evaluates for vault prolapse in any patient presenting with prolapse, because in many cases what appears to the unexperienced examiner to be a cystocele or rectocele is actually vault prolapse. This misdiagosis leads to improper or incomplete repair and usually causes shortening of the vagina because the apex is not suspended up to its natural position. In many cases vault suspensions are not completed by some surgeons secondary to being more advanced difficult surgical procedures that require experience and training and therefore add considerable time to the procedure in inexperienced hands.
Symptoms such as urinary frequency, urgency, nocturia, abnormal emptying of the bladder and pelvic pain that may occur with vault prolapse or after prolapse surgery without vault suspension are relieved many times following proper vault suspension as seen in the below sections.
Indications
Patients that experience vaginal vault prolapse often feel pressure, pain, protrusion and/or dyspareunia (painful intercourse). There are different degrees of prolapse from mild to severe. If the prolapse is moderate or severe (extending outside the vagina), serious problems such as urinary retention, dilated ureter or kidney and vaginal ulcers may occur and surgery is the next step.
Indications for Surgery
-
Moderate Prolapse
-
Severe Prolapse Causing Medical Problems
-
Failure of Pessary Management
-
Symptomatic Prolapse (pressure, pain)
-
Painful Intercourse
There are three many ways to perform vaginal vault suspension The most robust repair is laparoscopic sacrocolpopexy. Other options include sacrospinous ligament fixation and vaginal repair with mesh (Prolift TM). Mr Fayyad will discuss the surgical options after a complete physical examination and a discussion with the patient.
Laparoscopic sacrocolpopexy
The abdominal sacral colpopexy is one of the most successful operations for vaginal vault prolapse with excellent results. It involves suturing a synthetic mesh that connects and supports the vagina to the sacrum (tailbone). This procedure is complex in its nature and requires great expertise for a favorable outcome. Mr Fayyad has been performing the laparoscopic sacral colpopexy in the same manner as an open procedure with the exception of using a laparoscope over the past 5 years.
Advantages
By performing the sacral colpopexy laparoscopically, the vagina is repositioned to its anatomic position in a minimally invasive manner. Most surgeons perform this procedure through a large incision thus contributing to a longer recovery time. Our laparoscopic approach also allows us to incorporate additional laparoscopic procedures if needed.
Mr Fayyad can perform the laparoscopic sacral colpopexy in less time, less blood loss, smaller incisions and perform the surgery more precisely than by doing it through an open laparotomy. There are only very few centres in the country offering this procedure through the laparoscopic approach.
Surgical Technique for Laparoscopic Sacral Colpopexy
After placing the four small incision sites noted above (Figure 2) and then placing the access ports (Figure 3), the bowel is mobilized out of the deep pelvis and the sacrum (tailbone) is identified (Figure 4). The peritoneum over the sacrum (tailbone) is elevated (Figure 5) and then incised (Figure 6).
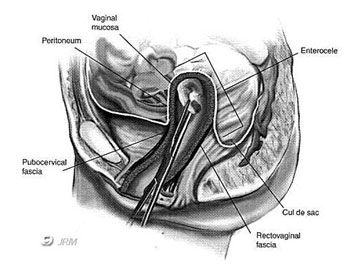
Figure 7b -- Vaginal vault (apex) : Probe holds vagina up from below
Figure 8 -- Y-shaped mesh
The long arm of the Y-mesh is then pulled up to the sacrum and subsequently attached. Figure 11 shows the placement of strong titanium staples into the sacrum, which will then be fixing the mesh. By attaching the mesh to the sacrum, the vagina is supported to the sacrum via a bridge of mesh between the vagina and sacrum. (Figure 12) The mesh is attached distally to the vagina (anterior & posterior) and proximally to the sacrum (Figure 14).
The peritoneum, which was originally incised and opened at the beginning of the operation, is now closed over the mesh (Figure 14). This part of the surgery does not add support to the surgery but is thought to decrease potential complications, like bowel obstruction and adhesions.
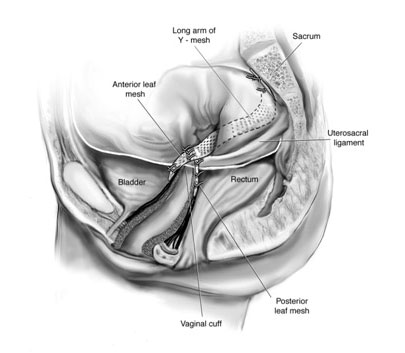
Figure 14- lateral view of mesh attached to the both anterior wall and posterior wall of vagina and then to the sacrum (tailbone).